Background
As the COVID-19 outbreak grew in early 2020, multiple U.S. health professional organizations and governmental agencies suggested suspending elective surgeries and non-essential medical procedures, including cancer screening. The Special Report for the latest Annual Report to the Nation on the Status of Cancer explores the relationship between cancer diagnoses in the U.S. and the disruptions caused by the first few months of the COVID-19 pandemic.
Researchers picked a sample of cancer sites to understand if COVID-19 affected new cancer diagnoses in the U.S. The studied cancer sites included ones with current screening guidelines: female breast, lung, and colorectal cancers. Other cancer sites included thyroid and prostate cancers, which are often detected incidentally, and pancreatic cancer, which has unfavorable outcomes.
By using cancer trends from 2015 to 2019, the researchers predicted the number of cancer diagnoses in 2020 and compared them against recorded diagnoses. One way to compare these numbers with each other is by taking a ratio, which divides one number by the other. In this case, the recorded number of cancer diagnoses in 2020 gets divided by the number of cancer diagnoses researchers predicted for 2020. If the ratio of these two numbers is 1, then the actual number of diagnosed cases is the same as the expected number of diagnosed cases. A number lower than 1 means there were fewer diagnosed cancer cases than expected.
All six cancer sites had a ratio of less than 1 at some point in 2020, meaning there were fewer diagnosed cases than expected for at least a couple of months.
Cancer Cases Diagnosed vs. Cancer Cases Expected in Early 2020
Decrease in Cancer Case Counts
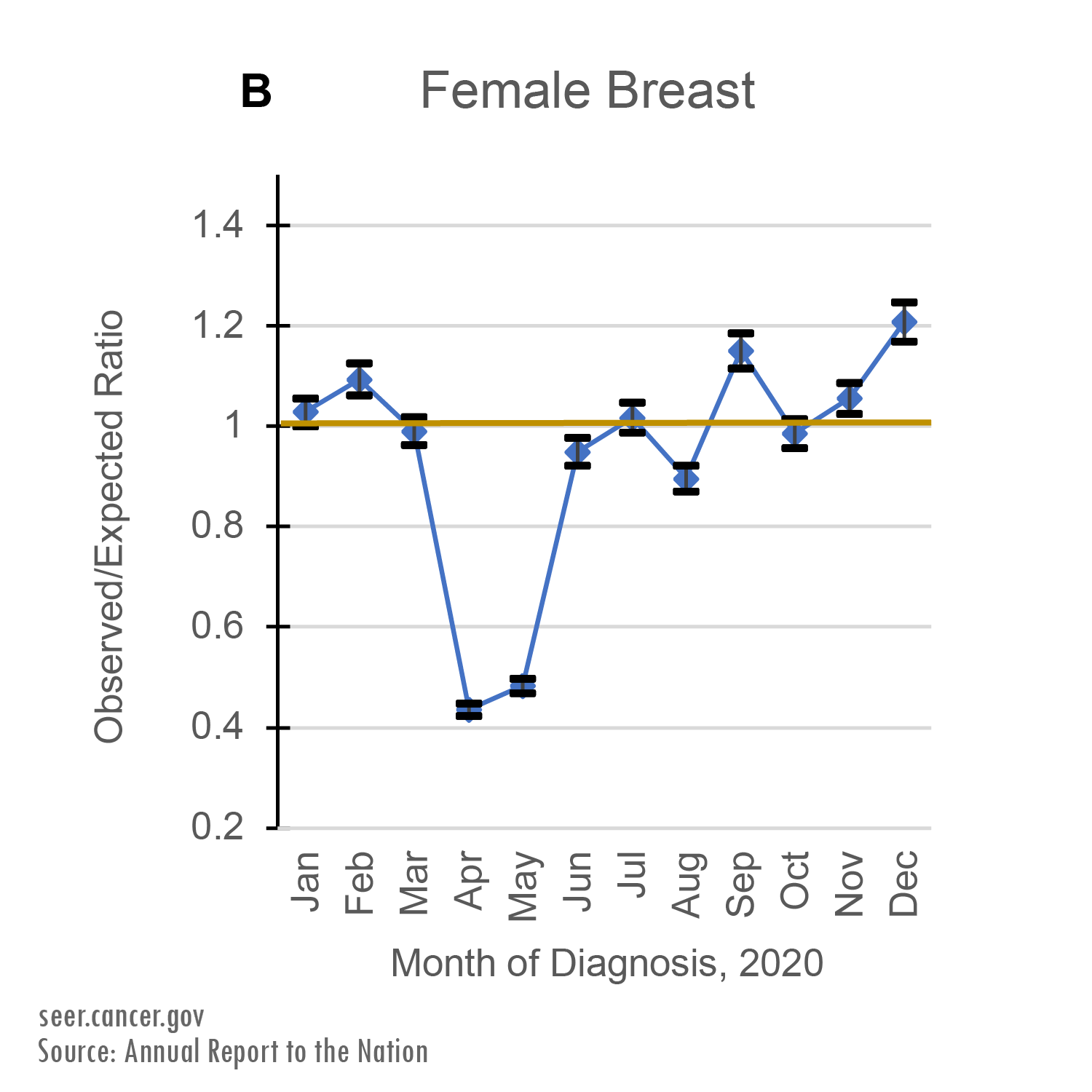
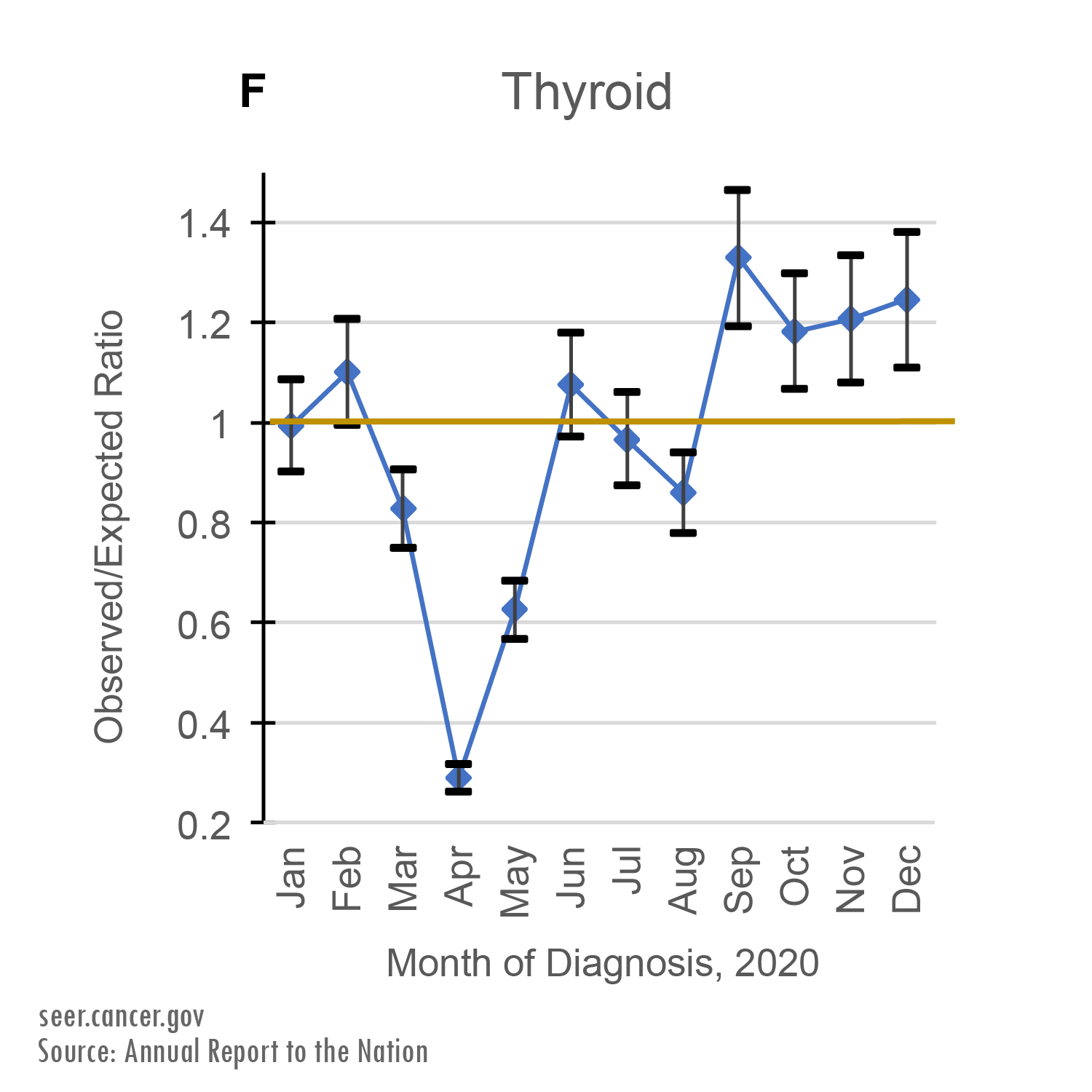
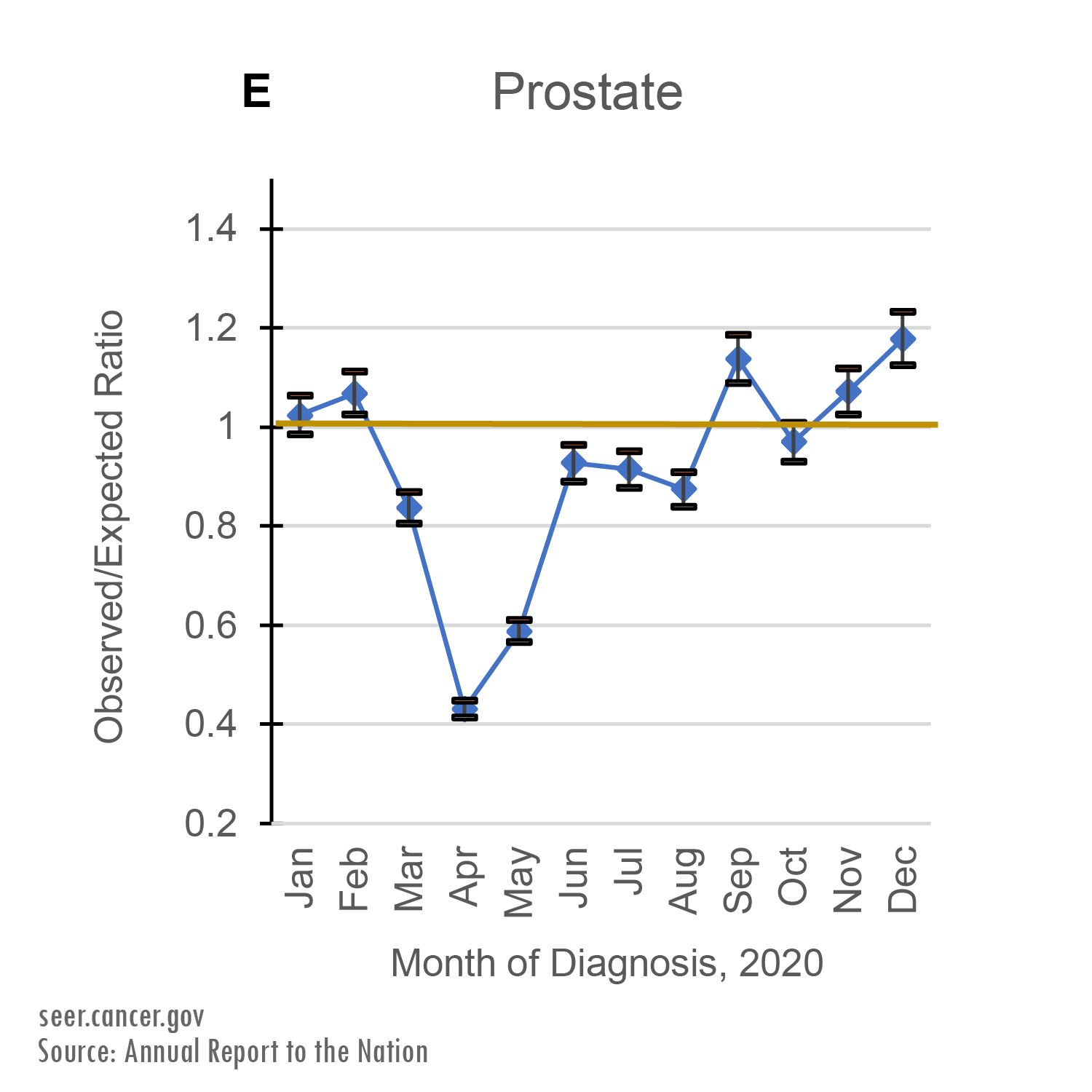
Between March and May of 2020, cancer registries recorded far fewer cancer cases than expected. April of 2020 had the lowest number of cancer diagnoses for all six cancer sites: breast, lung, colorectal, prostate, pancreatic, and thyroid.
Cancers with higher survival rates, like thyroid, prostate, female breast, and colorectal cancers, saw fewer than half of the expected number of diagnoses in April of 2020.
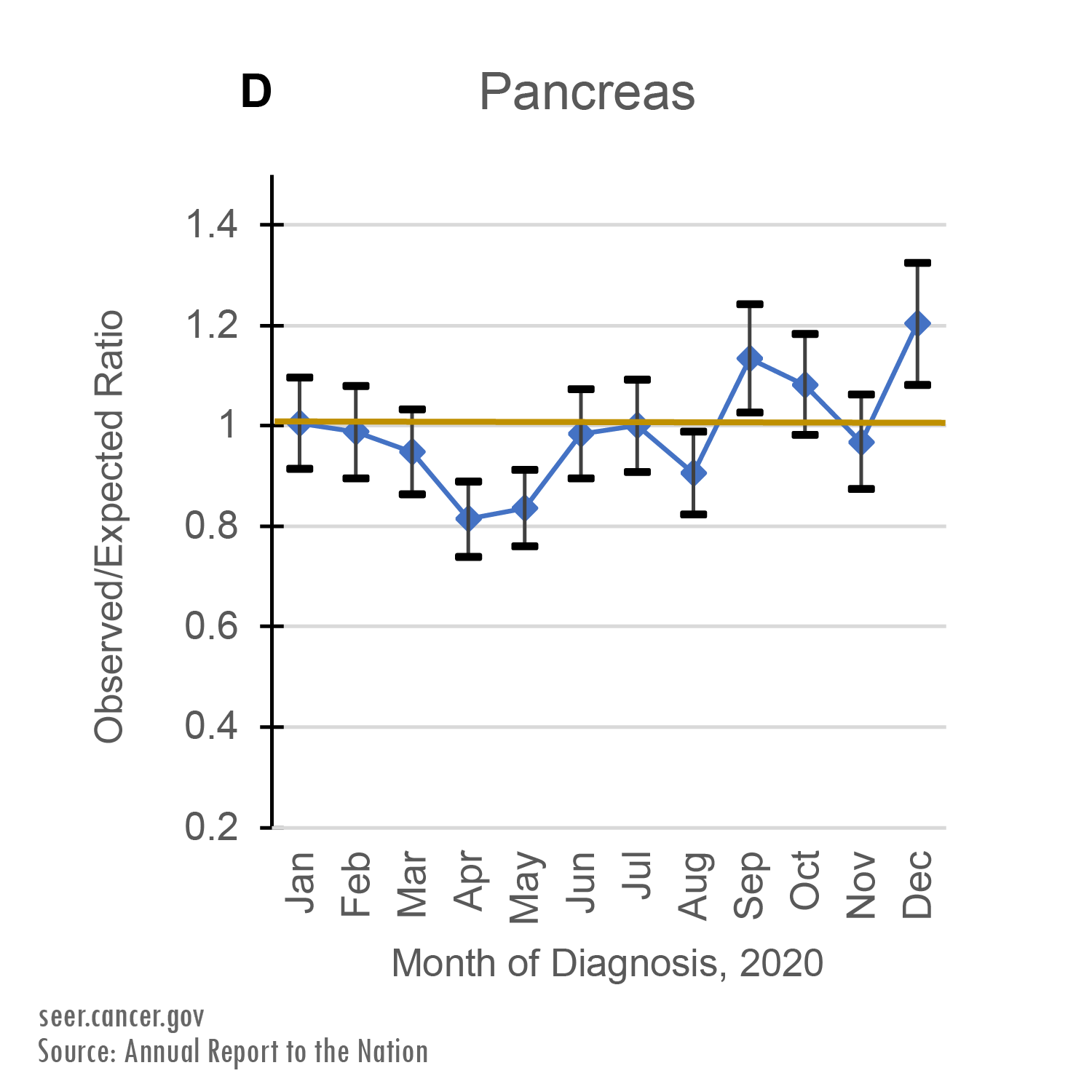
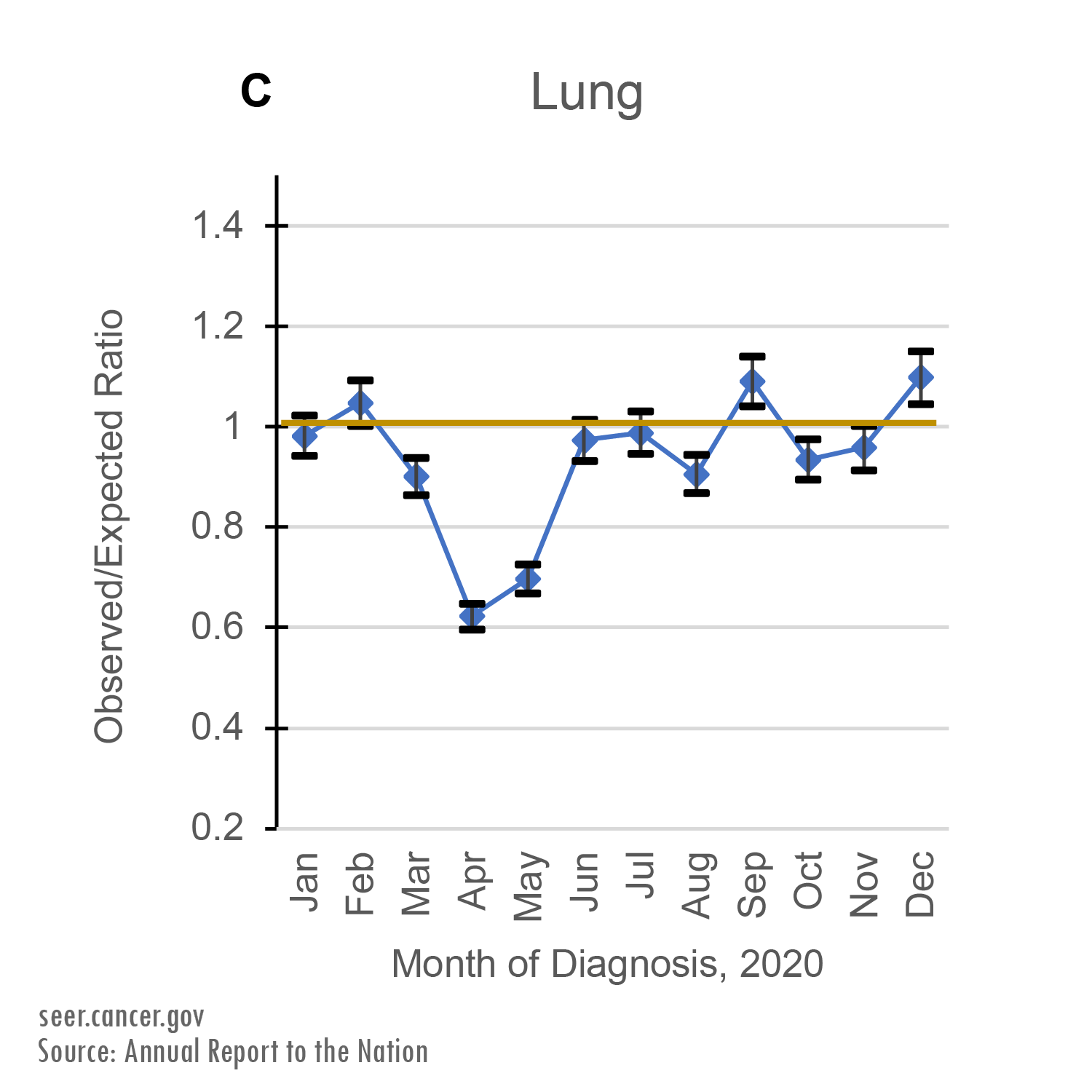
New pancreatic cancer cases fell by about 20% and new lung cancer cases fell by about 40% in April 2020. These two cancers have lower survival rates than the other four cancer types in this study.
These two cancers have lower survival rates than the other four cancer types in this study.
Asian and Pacific Islanders (API), compared to Whites, had a lower rate of cancer diagnoses across all sites except pancreatic cancer. Preexisting financial, linguistic, and cultural barriers to health care for this population likely worsened due to the COVID-19 pandemic.

By July 2020, diagnoses of all cancer types except prostate cancer had returned to the level we would have expected to see based on previous trends.
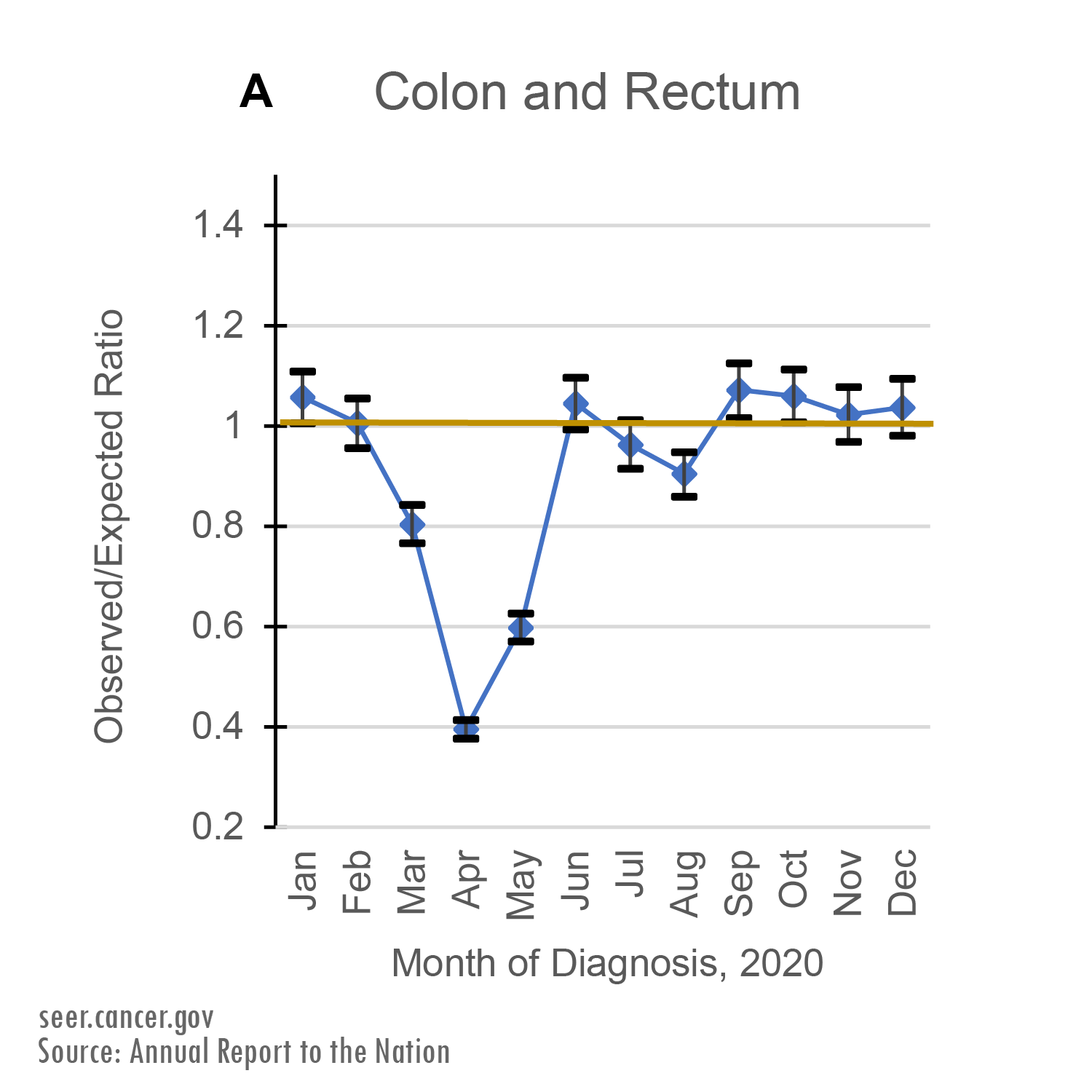
While the rate of new cancer diagnoses hovered around predicted levels in the second half of 2020, it did not make up for the drop seen between March and May. This pattern is most obvious in the graph for colorectal cancer diagnoses, below.
This pattern is most obvious in the graph for colorectal cancer diagnoses, below.
Decreases by Stage at Diagnosis
Rates of in situ or localized cancer diagnoses were lower than expected for all of the studied sites: colorectal (16.3% lower), prostate (14.8%), lung (14.7%), thyroid (11.8%), pancreas (9.9%), and female breast (9.0%).
Lower rates of new localized cancer cases can mean more people may not get diagnosed when the disease is the most treatable and survivable. Basically, thousands of people with cancer were not diagnosed as early as they would have been and therefore may have worse outcomes. There was not a sharp decrease in diagnoses of advanced cancers.
Fewer cancer screenings may explain the lower rates of new localized cancer cases. For example, female breast cancer screening rates dropped by 6% in 2020. This drop in cancer screening mirrors the 5% lower than expected rate of diagnoses for in-situ breast cancer, a disease stage where cancer cells have not spread beyond the original tumor. According to the report, getting back into routine health visits (including cancer screenings) can help patients get care earlier, when outcomes are best.
Decrease in Cancer Pathology Reports
When cancer is diagnosed, a lab note about the cancer's characteristics — also known as a pathology report — gets transmitted automatically to the cancer registry serving that region. The number of pathology reports decreased in 2020, suggesting lower rates of diagnoses are due to fewer in-person healthcare and screening visits instead of other factors like staff shortages. The smaller number of pathology reports also corroborated the lower rate of cancer diagnoses between April and May. Researchers continue to study the impact of the pandemic on cancer trends.

For more details about how the COVID-19 pandemic disrupted cancer diagnoses in the United States, read the full report here .
.